What does it mean for an agency to be Medicare-certified?
What is a Medicare-certified home health agency?
If a home health agency is “Medicare-certified” in that simply means that the agency is approved (i.e., certified) by Medicare and meets certain and specific federal health and safety requirements.
Let’s break this down…
Home health aides (HHA) can work in a variety of environments
Overwhelmingly though, aides work for home health agencies.
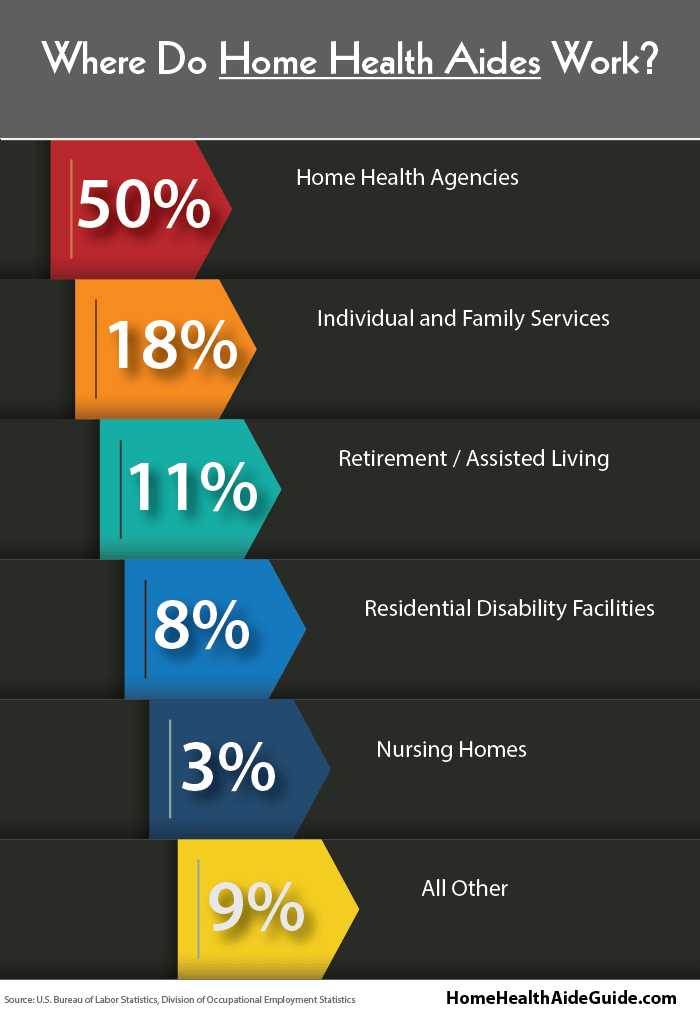
Home health agencies provide services to those who are homebound and need skilled nursing or therapy.
Example of services include nursing care and home care aide services (i.e., home health aides), as well as other services such as occupational therapy (OT), physical therapy (PT), speech therapy, and medical social services.
Medicare can pay for this care at home through Medicare-certified home health agencies.
What is Medicare?
Medicare is the federal government program that provides health care coverage for those:
- 65 years and older or
- under 65 and receiving Social Security Disability Insurance for a certain amount of time
The Centers for Medicare & Medicaid Services (CMS) operates Medicare and it is funded in part by Social Security and Medicare taxes – too much information for this discussion…
Once an individual becomes Medicare-eligible and enrolled, he/she can choose the plan that best suits them.
Conditions to receive Medicare home health benefits in
To be eligible for Medicare home health benefits, an individual must meet all of these conditions:
- Homebound: unable to leave home without considerable effort or without the aid of another person or a device such as a wheelchair or a walker
- Doctor Certified: being in need of intermittent occupational therapy, physical therapy, skilled nursing care and/or speech-language therapy
- Meeting with a medical professional no more than 90 days before or 30 days after the start of home health care
- Under a plan of care that a doctor established and reviews regularly.
- Medicare has approved the home health agency caring for you
Most home health agencies are Medicare approved; this means they can provide services that will be reimbursed by Medicare.
How the Medicare-certified status of an agency affects home health aides
MATTER OF LAW
Medicare-certified home health agencies can only hire and employ home health aides who have been trained and passed a competency evaluation – that is, they need to certified.
Agency requirements to be considered Medicare-certified
There are more than 11,000 home health agencies in the US.
Matter of fact: a whopping 99% of home health agencies are Medicare certified.
The small percentage of agencies that are not certified may be so for a variety of reasons. Perhaps, some don’t provide the breadth of services that Medicare requires (e.g., skilled nursing care) and some may only accept private pay clients.
Home health agencies that are Medicare approved (aka certified) can provide services that will be reimbursed by Medicare.
They have gone through the time and expense of getting certified and clearly think it is worth it in order to build their business and be profitable.
This is a lot to take in, but bear with us.
Here are the home health agency requirements to be considered Medicare-certified.
The agency must:
- Provide skilled nursing services and at least one of the following other services: physical therapy speech language pathology, or occupational therapy medical social services, or home health aide services in a place of residence used as a patient’s home
- Has policies established by a group of professionals who are associated with the agency, including one or more physicians and one or more registered professional nurses, to govern the services;
- Provide for supervision of these services by a physician or registered professional nurse; and maintains clinical records on all patients;
- Be licensed pursuant to State law, or has approval as meeting the standards established for licensing by the State or locality;
- Have a plan and budget for institutional planning;
- Meet the federal requirements in the interest of the health and safety of individuals who are furnished services by the agency; and
- Meet any additional requirements the federal government finds necessary for the effective and efficient operation of the program.
Only when all of the above is satisfied can the agency offer home health care to Medicare qualified recipients – and the care can only be provided by certified home health aides (and, of course, other licensed professionals such as registered nurses).
Agency Conditions of Participation (CoPs)
As you have guessed, it does not stop there.
There are minimum health and safety standards a home health agency must meet in order to participate in the Medicare and Medicaid programs.
These standards fall under what is commonly called: “Conditions of Participation (CoPs)”.
CoPs are federal regulations with which home health agencies must comply in order to receive funding from Medicare and Medicaid programs.
The CoPs requires that the agency:
- Protect and promote the rights of each individual under its care;
- Disclose ownership and management information;
- Not use as a home health aide (on a full-time, temporary, per diem, or other basis) any individual to provide items and services, unless the individual has completed a training and competency evaluation program that meets minimum standards, and is competent to provide such items and services;
- Operate and provide services in compliance with all applicable Federal, State, and local laws and regulations;
- Operate and provide services in compliance with accepted professional standards and principles which apply to professionals providing items and services for the HHA;
- Include an individual’s plan of care as part of the clinical record; and
- Comply with requirements relating to maintaining written policies and procedures respecting advance directives
The law states the requirements of home health agencies to hire only certified home health aides.

In Summary
Most home health agencies are Medicare-certified which means they can only employ home health aides who have been trained and passed a competency exam – they must be certified.

